Formerly known as Gain Life
AI
& Automation for P&C
Connecting experience to outcomes
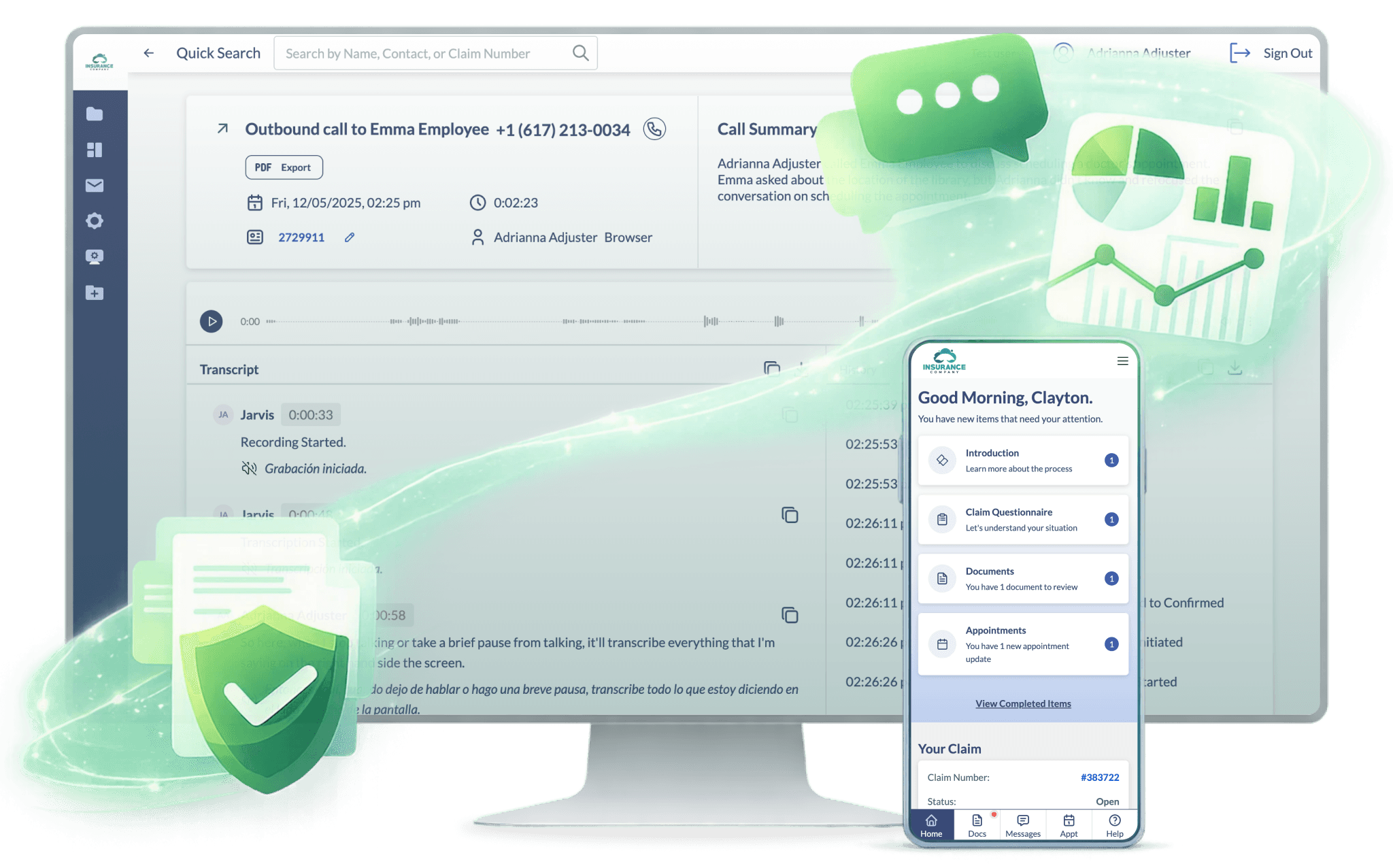
Crosstie helps carriers, TPAs, and self-insureds resolve claims faster, reduce costs, and improve the experience for everyone involved — through a modular platform that connects workflows across documents, voice, communication, and claimant engagement.
Start with a single workflow or deploy across the entire claims and service lifecycle.
Crosstie helps carriers, TPAs, and self-insureds resolve claims faster, reduce costs, and improve the experience for everyone involved — through a modular platform that connects workflows across documents, voice, communication, and claimant engagement.
Start with a single workflow or deploy across the entire claims and service lifecycle.

Trusted by companies that care about who they serve











Start with the problem you need to solve today
Whether it's summarizing medical records, identifying time limit demands, automating intake, summarizing claim files, or handling inbound calls — start with the workflows slowing you down most and expand from there.
Customer Communication
Guide customers every step of the way
Configurable rules provide clear, personalized guidance throughout any process, reducing confusion and keeping everyone on track.




Customer Communication
Guide customers every step of the way
Configurable rules provide clear, personalized guidance throughout any process, reducing confusion and keeping everyone on track.








Predictive Insights
Spot problems before they happen
AI monitors workflows 24/7, flagging potential delays or issues before they impact outcomes, so your team can resolve problems proactively.



Predictive Insights
Spot problems before they happen
AI monitors workflows 24/7, flagging potential delays or issues before they impact outcomes, so your team can resolve problems proactively.
Decision Support
Suggest smart solutions for faster resolutions
AI-powered suggestions and alerts guide teams to faster resolutions using proven strategies, improving efficiency across all workflows.




Decision Support
Suggest smart solutions for faster resolutions
AI-powered suggestions and alerts guide teams to faster resolutions using proven strategies, improving efficiency across all workflows.


Why forward-thinking organizations choose Crosstie
A configurable, end-to-end platform built specifically for insurance workflows.

One platform across the entire claim and service lifecycle
From intake to settlement, in any language. One platform replaces multiple vendors, reducing complexity and costs.

One platform across the entire claim and service lifecycle
From intake to settlement, in any language. One platform replaces multiple vendors, reducing complexity and costs.

Security you can trust
Role-based permissions and guardrails ensure sensitive data is always protected and compliant, so every user and agent sees only what they should.

Security you can trust
Role-based permissions and guardrails ensure sensitive data is always protected and compliant, so every user and agent sees only what they should.

Configurable to how your business actually operates
Adapt workflows, rules, and communications as your needs change. No IT bottlenecks. Go live in 4-6 weeks.

Configurable to how your business actually operates
Adapt workflows, rules, and communications as your needs change. No IT bottlenecks. Go live in 4-6 weeks.

Works with your existing systems
Integrates with claims, policy, and RMIS platforms. No rip-and-replace required, just better ROI from the systems you already use.

Works with your existing systems
Integrates with claims, policy, and RMIS platforms. No rip-and-replace required, just better ROI from the systems you already use.

Enterprise-proven at scale
Trusted by some of the largest carriers, TPAs, and self-insureds. Handles enterprise volumes while cutting cycle times and boosting satisfaction.

Enterprise-proven at scale
Trusted by some of the largest carriers, TPAs, and self-insureds. Handles enterprise volumes while cutting cycle times and boosting satisfaction.
Solve the workflows that slow you down
Prioritize the highest-friction work, and automate what slows your team down first.
1.
Guide claimants and policyholders every step of the way
Automatically deliver required actions, updates, and reminders—reducing confusion, missed tasks, and inbound calls.
2.
Identify delays and risks before they escalate
Analyze claim activity across documents, messages, and calls to surface delays, missed steps, and early risk signals.
3.
Recommend next-best actions to resolve claims faster
AI-powered suggestions and alerts guide teams to faster resolutions using proven strategies, improving efficiency across all workflows.
Customer Outccomes
Proven results that matter
Measurable results across carriers, TPAs, and self-insureds.
%
Identify claims headed for litigation 3+ weeks early
Automatically trigger early interventions so teams can resolve issues before they escalate.
+
Hours saved per adjuster per week
Faster document signing, reduced phone tag, fewer questions, and seamless multilingual communication free up time for higher-value work.
%
Reduction in total direct claim costs
Independently analyzed customer data shows statistically significant cost savings of 25% for medical-only claims and $18,997 per complex lost-time claim.
x
Higher engagement than standard portals
Claimants and policyholders get the seamless digital experience they expect, leading to faster resolutions and better satisfaction scores.
Wegmans Food Markets
“Jarvis by Crosstie has been a game-changer for our Claims Administration team and life-changing for our injured employees. Our team has more prescriptive data to be able to help our injured employees recover more quickly and have a better quality of life while doing so. The technology allows our team to focus more on hospitality, getting injured employees what they need before they know they need it. Our injured employee engagement rate with the app is 71.76%, and the satisfaction rate is 9/10, or 88%!"
B
Brian Trick, Director of Employee Health and Claims Services
FFVA Mutual
“Through direct contact with the injured worker via their smart device in their native language, TRUclaim Solution, powered by Crosstie, shortens the claims lifecycle with fast, accurate communication and speedy delivery of benefits."
A
Adrienne Kaltenschnee, Supervisor Claims Adjusters & Software Operations
Johns Eastern Company, Inc. - A Davies Company
“Johns Eastern is thrilled to partner with Crosstie in providing a modern means of communication for injured workers and our staff. Injured workers are able to chat with the adjuster or nurse case manager, submit forms, look up indemnity payments and manage medical appointments all from their personal computer, tablet, or phone. We appreciate Crosstie’s continued involvement to improve processes and ensure that our participation rate consistently increases each month."
A
Alice Wells, Executive Director of TPA Operations
Customer Outccomes
Proven results that matter
Measurable results across carriers, TPAs, and self-insureds.
%
Identify claims headed for litigation 3+ weeks early
Automatically trigger early interventions so teams can resolve issues before they escalate.
+
Hours saved per adjuster per week
Faster document signing, reduced phone tag, fewer questions, and seamless multilingual communication free up time for higher-value work.
%
Reduction in total direct claim costs
Independently analyzed customer data shows statistically significant cost savings of 25% for medical-only claims and $18,997 per complex lost-time claim.
x
Higher engagement than standard portals
Claimants and policyholders get the seamless digital experience they expect, leading to faster resolutions and better satisfaction scores.
Wegmans Food Markets
“Jarvis by Crosstie has been a game-changer for our Claims Administration team and life-changing for our injured employees. Our team has more prescriptive data to be able to help our injured employees recover more quickly and have a better quality of life while doing so. The technology allows our team to focus more on hospitality, getting injured employees what they need before they know they need it. Our injured employee engagement rate with the app is 71.76%, and the satisfaction rate is 9/10, or 88%!"
B
Brian Trick, Director of Employee Health and Claims Services
FFVA Mutual
“Through direct contact with the injured worker via their smart device in their native language, TRUclaim Solution, powered by Crosstie, shortens the claims lifecycle with fast, accurate communication and speedy delivery of benefits."
A
Adrienne Kaltenschnee, Supervisor Claims Adjusters & Software Operations
Johns Eastern Company, Inc. - A Davies Company
“Johns Eastern is thrilled to partner with Crosstie in providing a modern means of communication for injured workers and our staff. Injured workers are able to chat with the adjuster or nurse case manager, submit forms, look up indemnity payments and manage medical appointments all from their personal computer, tablet, or phone. We appreciate Crosstie’s continued involvement to improve processes and ensure that our participation rate consistently increases each month."
A
Alice Wells, Executive Director of TPA Operations
Customer Outccomes
Proven results that matter
Measurable results across carriers, TPAs, and self-insureds.
%
Identify claims headed for litigation 3+ weeks early
Automatically trigger early interventions so teams can resolve issues before they escalate.
+
Hours saved per adjuster per week
Faster document signing, reduced phone tag, fewer questions, and seamless multilingual communication free up time for higher-value work.
%
Reduction in total direct claim costs
Independently analyzed customer data shows statistically significant cost savings of 25% for medical-only claims and $18,997 per complex lost-time claim.
x
Higher engagement than standard portals
Claimants and policyholders get the seamless digital experience they expect, leading to faster resolutions and better satisfaction scores.
Johns Eastern Company, Inc. - A Davies Company
“Johns Eastern is thrilled to partner with Crosstie in providing a modern means of communication for injured workers and our staff. Injured workers are able to chat with the adjuster or nurse case manager, submit forms, look up indemnity payments and manage medical appointments all from their personal computer, tablet, or phone. We appreciate Crosstie’s continued involvement to improve processes and ensure that our participation rate consistently increases each month."
A
Alice Wells, Executive Director of TPA Operations
FFVA Mutual
“Through direct contact with the injured worker via their smart device in their native language, TRUclaim Solution, powered by Crosstie, shortens the claims lifecycle with fast, accurate communication and speedy delivery of benefits."
A
Adrienne Kaltenschnee, Supervisor Claims Adjusters & Software Operations
Wegmans Food Markets
“Jarvis by Crosstie has been a game-changer for our Claims Administration team and life-changing for our injured employees. Our team has more prescriptive data to be able to help our injured employees recover more quickly and have a better quality of life while doing so. The technology allows our team to focus more on hospitality, getting injured employees what they need before they know they need it. Our injured employee engagement rate with the app is 71.76%, and the satisfaction rate is 9/10, or 88%!"
B
Brian Trick, Director of Employee Health and Claims Services
Get Started with Crosstie
Ready to modernizeyour insurance operations?
Crosstie helps insurers automate workflows, reduce cycle times, and improve customer outcomes. See how leading carriers, TPAs, and self-insured organizations are transforming their operations.

Get Started with Crosstie
Ready to modernizeyour insurance operations?
Crosstie helps insurers automate workflows, reduce cycle times, and improve customer outcomes. See how leading carriers, TPAs, and self-insured organizations are transforming their operations.

Get Started with Crosstie
Ready to modernizeyour insurance operations?
Crosstie helps insurers automate workflows, reduce cycle times, and improve customer outcomes. See how leading carriers, TPAs, and self-insured organizations are transforming their operations.

